Cryoablation of Renal Tumors
Cryoablation of Renal Tumors
There are many ways to treat renal tumors apart from surgery. Radiofrequency ablation (RFA) has been used for renal tumors, especially in single kidneys or in patients at high risk for surgery / anesthesia, for more than two decades now. Cryoablation is now an alternative.
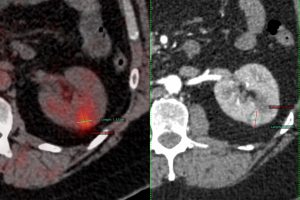
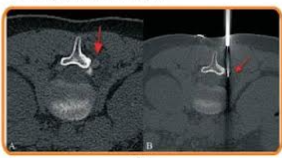
As with any ablative technique, the cryoprobe is guided into the tumor using CT and CT fluoroscopy and then depending on the size, the ablation is performed for a specific period of time. While cryoablation has been used for larger than 4 cm lesions, mainly for palliation, it is best suited for < 4 cm sized lesions, especially in single kidneys (Fig. 1), where the extent of renal damage can be controlled and where the extent of nephron sparing is better than with surgery.
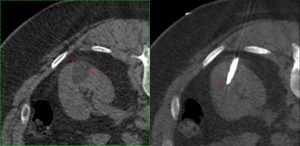
Cryoablation is ideal for renal tumors, mainly because the iceball (Fig. 2) and hence the ablation zone can be much better defined than other thermal ablative techniques such as RFA or microwave. The procedure is usually quite simple and straightforward, done without sedation, unless the patient is uncomfortable, in which case, conscious sedation is used.
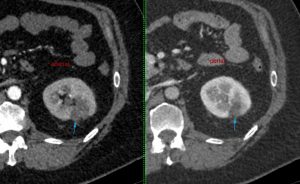
Though, a randomized controlled trial has not yet been performed, observational data shows good efficacy and accuracy of cryoablation (Fig. 3).
At a glance:
- Cryoablation is an emerging technique for small renal tumors
- The best indication at present is < 4 cm tumors either in single kidneys or in patients at high risk for surgical / anesthetic complications.