Comparing Treatment Options for Osteoid Osteoma: Why Radiofrequency Ablation Stands Out
Osteoid osteoma is a benign bone tumor that commonly affects young individuals, causing persistent pain and discomfort. Effective treatment options are essential to alleviate symptoms and improve the quality of life for affected individuals. While several treatment modalities exist, this blog post will focus on comparing these options and highlighting why radiofrequency ablation (RFA) stands out as a superior choice for managing osteoid osteoma.
Understanding Osteoid Osteoma:
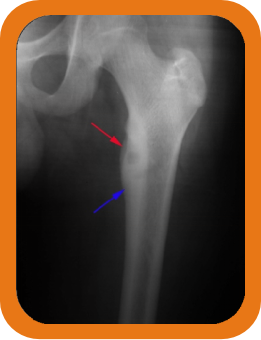
Osteoid osteoma typically manifests as localized pain that worsens at night and is partially relieved by nonsteroidal anti-inflammatory drugs (NSAIDs). This condition occurs when a small tumor, usually less than 2 cm in diameter, develops within the bone cortex. Osteoid osteoma most commonly affects the long bones of the lower extremities, such as the femur and tibia, but it can occur in any bone in the body.
Treatment Options:
Nonsteroidal Anti-inflammatory Drugs (NSAIDs):
NSAIDs are often prescribed as the first line of treatment for osteoid osteoma. While they can provide temporary pain relief, they do not address the underlying tumor. Long-term use of NSAIDs can also lead to potential side effects such as gastrointestinal problems, kidney damage, and cardiovascular complications.
Observation:
In some cases, small osteoid osteomas may be monitored without active intervention. This approach is typically reserved for asymptomatic patients with lesions that are unlikely to cause significant pain or complications. However, it’s important to note that this strategy does not resolve the tumor and may result in prolonged discomfort.
Surgical Excision:
Surgical excision involves removing the tumor through open surgery. While this method effectively eliminates the tumor, it has several disadvantages. Surgery is an invasive procedure that carries risks of complications, including infection, scarring, and prolonged recovery time. Additionally, it may require general anesthesia, which presents its own set of risks.
Radiofrequency Ablation (RFA):
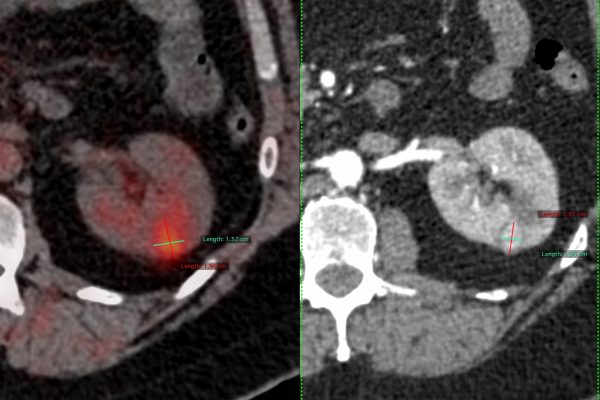
RFA has emerged as a minimally invasive and highly effective treatment option for osteoid osteoma. This technique involves inserting a thin needle into the tumor under image guidance, such as computed tomography (CT) or ultrasound, and delivering high-frequency electrical currents to heat and destroy the tumor cells. RFA can be performed under local anesthesia, reducing the risk associated with general anesthesia.
Why Radiofrequency Ablation Stands Out:
High Success Rate:
Radiofrequency ablation has demonstrated a high success rate in treating osteoid osteoma, with studies reporting success rates of over 90%. This non-invasive procedure effectively destroys the tumor, providing long-lasting pain relief and improving overall quality of life.
Minimally Invasive:
Compared to traditional open surgery, RFA is a minimally invasive procedure that requires only a small incision for needle insertion. This results in shorter recovery time, reduced postoperative pain, and decreased risk of complications such as infection or scarring.
Preserves Healthy Tissue:
Radiofrequency ablation precisely targets the tumor, minimizing damage to surrounding healthy tissue. This focused approach helps preserve bone strength and functionality while eliminating the source of pain.
Outpatient Procedure:
RFA is often performed on an outpatient basis, allowing patients to return home on the same day. This eliminates the need for an extended hospital stay and reduces healthcare costs.
Minimal Side Effects:
Radiofrequency ablation is associated with minimal side effects. Some patients may experience temporary discomfort at the needle insertion site or mild swelling, which typically resolves within a few days. The risks and complications associated with this procedure are significantly lower compared to surgical excision.
Conclusion:
When comparing treatment options for osteoid osteoma, radiofrequency ablation clearly stands out as a superior choice. Its high success rate, minimally invasive nature, preservation of healthy tissue, outpatient procedure, and minimal side effects make it an attractive option for patients seeking effective and efficient pain relief. However, it is important for patients to consult with their healthcare providers to determine the most appropriate treatment option based on individual circumstances and preferences.